In the health care industry, there are many legal arrangements that help practices operate smoothly and compliantly. The Management Services Agreement (“MSA”) is a critical document used in Management Services Organization (“MSO”) models. But what exactly is an MSA, and how does it work? Let’s dive into the essentials.
Understanding the Basics of an MSA
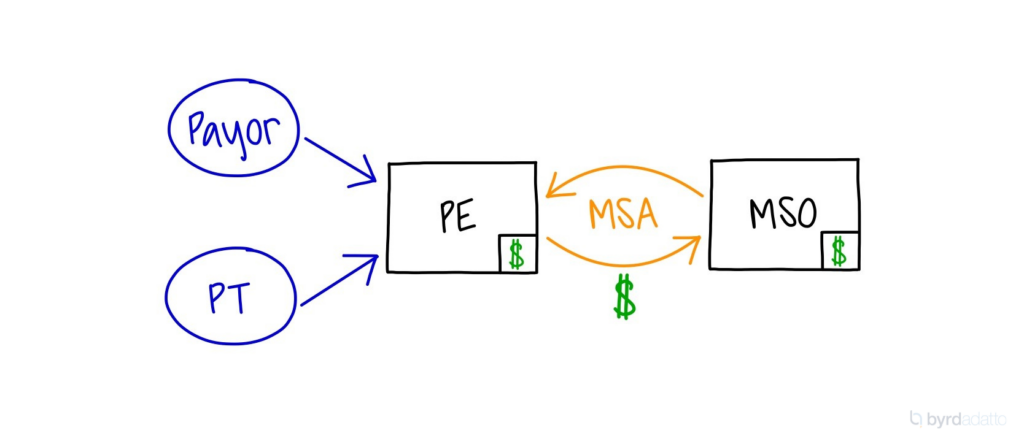
A Management Service Agreement (MSA) is a contract between a medical practice and an MSO. It details how the MSO provides non-clinical administrative and management services to the medical practice. Such services can include human resources, billing and collections, marketing, facilities management, and information technology support. The purpose of the arrangement is to allow the medical providers to focus on delivering patient care and the clinical side of operations while the MSO handles the business side of operations.
The separation of responsibilities is particularly important in health care where compliance with federal and state regulations is critical. The medical practice via the physician, physician assistants, nurse practitioners must be responsible for the medical decision making and delegating to the applicable staff. The MSO cannot insert its opinion on any medical decision making. The MSA should reflect this in addressing the roles and responsibilities of each of the parties.
Key Elements of an MSA
While the specifics of an MSA can vary depending on the parties involved, most agreements share some common elements:
Scope of Services
The MSA clearly defines the administrative and management services the MSO will provide to or on behalf of the medical practice.
Compensation Structure
The MSA details how the MSO will be compensated for its services rendered. Depending on the applicable law, compensation can be a flat fee, a percentage of revenues, or another agreed-upon method. Importantly, the compensation must comply with federal and state laws, such as the federal Anti-Kickback Statute and state fee-splitting and corporate practice of medicine doctrines.
Termination
The MSA addresses termination, specifying the conditions under which either party can end the agreement.
Compliance with Laws
The MSA complies with applicable laws and regulations to avoid legal issues, including those governing fee-splitting and the corporate practice of medicine. As mentioned above, one primary way is to clearly reflect the appropriate roles and responsibilities of both the MSO and medical practice.
Why MSAs Are Important
MSAs are essential for structuring compliant and efficient relationships between MSOs and medical practices. They help clarify the roles and expectations of both parties, reducing the likelihood of disputes. Additionally, they ensure that administrative functions are managed professionally, allowing physicians to focus on patient care.
However, MSAs must be carefully developed to avoid regulatory pitfalls. An improperly structured MSA can lead to significant legal risks. Similarly, poorly managed MSO arrangements can lead to compliance failures.
Common Misconceptions About MSAs
One common misconception is that MSAs are interchangeable with Medical Director Agreements or even unnecessary, but it is important to be aware that they serve different purposes. A Medical Director Agreement typically focuses on the clinical oversight and supervision provided by a physician, whereas a MSA pertains to non-clinical administrative services.
Another misconception is that physicians can take a hands-off approach to the medical practice’s operations when it is a party to a MSA. Physicians must remain actively involved in clinical decision-making and compliance matters. Absentee physicians allow for non-physicians to start making medical decisions and operate outside their scope, and the medical practice failing to meet the standard of care and drift out of compliance. Such actions expose the physician’s medical license to potential medical board investigations.
Avoid Legal Pitfalls
To prevent potential legal issues, you should:
- Work with experienced health care attorneys to draft or review MSAs to ensure compliance with your state rules.
- Make sure the way you operate your business aligns with the MSA. Having the MSA is a step towards compliance (i.e. the form), but the way the business operates and interacts is just as important (i.e. the substance). You need to make sure both are saying and doing the same thing.
- To avoid compliance drift, regularly audit the services provided by the MSO to ensure the MSO model is operating in accordance with state rules and regulations.
- Understand the state-specific rules regarding the corporate practice of medicine, and that each state can be different. Also know that the health care industry is constantly changing so staying up to date to make any necessary changes.
Overlooking such considerations can have dire consequences, potentially jeopardizing a medical practice’s viability.
ByrdAdatto Can Develop Your Management Services Agreement
A well-structured MSA can be a valuable tool for medical practices seeking to optimize their operations. By clearly defining roles, responsibilities, and compensation, a MSA allows medical professionals to focus on what they do best: caring for patients. However, these agreements must be approached with careful planning and legal expertise to ensure compliance and avoid costly mistakes.
At ByrdAdatto, we help practices incorporate compliant MSAs into their practice. Our legal team can provide further guidance on your state’s regulations for MSAs. If you want to learn more about structuring a compliant MSO model, contact ByrdAdatto.
